If you remember the movie
“Love Actually”, the opening scene was at an airport where, as the narrator says, the most sincere kind of love can be perceived. There’s more to that----the hospital. I have been rotating for three weeks in Internal Medicine and never did I see such form of sincere love as that of the love I have seen among my patients and their family members—fathers, mothers, sisters, brothers, husbands and children.
Patient A.M. is a 48 year old female, married with one child, and was diagnosed to have colon cancer earlier this year. She underwent colon resection and had been on six cycles of chemotherapy until three months ago when a palpable mass was noted in her abdomen. The mass have been growing gradually and was seen by her medical oncologist but they cannot rule out whether the mass was a primary growth or a metastasis from her previous colon malignancy. On my first week of rotation, November 4 to be exact, she was admitted at the ER due to
“agitation”. She was restless and agitated, shouting at her husband and her brother who accompanied them to PGH. The physician on duty considered the increased levels of toxins in her body as a cause of her behavioral changes
(uremic encephalopathy), that’s why she was admitted under our service. Apparently, her abdominopelvic mass impinges on both of her ureters which causes her minimal urine output, hence, accumulation of toxins in her body. She underwent series of hemodialysis and marked improvement of her sensorium was noted. She was herself again. We referred her to different services such as OB-GYN, Med Onco, Urology and General Surgery for possible intervention to relieve her of her symptoms. Laboratory work ups were done, her abdominal CT scan showed an ovarian new growth which obstructed the pathway of her urine that led to chronic kidney failure resulting to all her symptoms. Since we have treated the encephalopathy, we were contemplating on transferring her to other services particularly the GYN-Oncology. While waiting for the response of other services, I visit her everyday at her bedside to ask on the progress or relief of her symptoms. Her husband and her brother were always there too while I pass by for a quick chitchat, they never failed to meet my patient’s needs. What I appreciated most was that they were very aggressive; they comply with ALL the laboratories we request no matter how costly it would seem for them. I never had any difficulty facilitating her labs because the husband and the brother were always on the go. She was my patient for more than two weeks and despite the asymmetry of her face caused by congenital neck muscular problem
(torticollis), she’s always ready for a warm smile as she slowly raises her hand to wave at me. I always feel important whenever I visit her because she stops whatever she does saying
“Uy, ayan na si doktora”. She always tells me how she feels about her illness, her high hopes and her fears. While I can only offer my listening ears and an occasional light encouraging rub on her back, she would usually hold my hand tight while she complains how awful she feels about her edematous feet and her abdominal mass which frequently cause her pain.
After more than two weeks, her encephalopathy had resolved, all labs were done, the decision now lies in the hands of OB-GYN. They did a transvaginal and abdominal ultrasound and saw the strongly adherent mass on the abdominal wall, it would be a difficult operation and the result may be unfavorable, the OB-GYN senior resident said. They can only do mass debulking and staging, which, obviously is already stage 4. They presented the option to the patient, they can do mass debulking followed by chemotherapy but the prognosis is still bad, OR we refer them to the Hospice for counseling and terminal illness care. After a lengthy discussion among the family, they decided to just do home care. My patient was crying while she was telling me “Doktora, hindi na raw ako gagaling. Wala rin namang mangyayari, gagastos pa kami. Uuwi na lang po kami”. I do not know what sympathizing words to say. I only stood beside her and held her hand tightly, trying to utter comforting words (of which, I am very bad at) and reminded her how lucky she is that her husband and her brother never left her side. I reminded her of the love her husband had shown and given her. That, I said, makes her the luckiest person on earth because despite her illness, she was loved sincerely by her family.
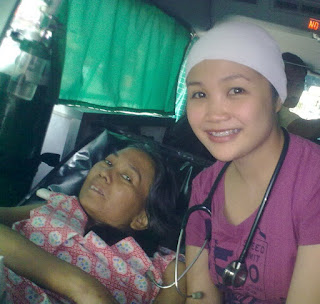
They already went home yesterday, and because I got so very busy at the other ward tending to another dying patient, I lacked time visiting her. Besides, I suck at goodbyes and I hate being attached to patients because it’s not just right for people like us who see dying and hopeless people every single day. But with this patient, it’s different. I noticed her empty bed on my way to the interns’ callroom and felt a pinch in my heart. I had many unsaid goodbyes in the past and this patient is an addition to my semi-regrets. Suddenly, I heard her brother calling me asking where he can possibly find the Nephro Fellow who attended to them. I asked the whereabouts of my patient and told me she was at the ambulance outside. I hurriedly ran outside, saw the parked ambulance and peeped behind the green curtain. Her husband swung open the back door and saw my patient lying on the stretcher while weeping and saying “Doktora, hindi ko po kayo makakalimutan. Maraming salamat po.” I jokingly told her not to cry because she got me teary-eyed as well. I pacified her by telling her to have her picture taken with me using my mobile phone. Her torticollis made her unable to smile normally but she still attempted to give me a good one.
I will never forget this patient and her family who stood by her from the beginning all the way until all the possible means were exhausted. Through her husband, I saw the picture of what true love is. I can only pray that he will never get tired of taking care of her until the very end. There may not be a cure for her disease but when the time comes that she has to leave this world, I know that her heart is full of love and contentment by what her family has given her. That, for me, is true love.
Photo with my patient inside the ambulance right before they went home against medical advise.